Why Reassurance Makes OCD Worse
Even when it feels like the kindest, most logical thing to do
Written by Armaan Raheja, Founder of breakOCD | Clinically reviewed by Jehanzeb Baldiwala (MA, Psychology), Psychologist, Mumbai
In This Article
- What Reassurance Seeking Actually Is
- Why Reassurance Feels So Good in the Moment
- The Reassurance Cycle in OCD
- How Reassurance Seeking Shows Up Across OCD Themes
- The Indian Family Dynamic and Reassurance
- The Difference Between Support and Reassurance
- Why the Brain Keeps Asking
- What Actually Helps: Responding Differently
- Frequently Asked Questions
Reassurance feels like relief. But in OCD, every time you seek it, you are quietly telling your brain that the fear was real and the threat was worth responding to. That lesson is very hard to undo.
If you live with OCD, you have probably experienced this pattern more times than you can count. A frightening thought arrives. Anxiety spikes. You ask someone a question, search for an answer online, or replay the situation in your mind until it feels resolved. The anxiety drops. You feel calmer. For a moment, you are okay.
Then the doubt comes back.
This is the reassurance cycle, and it is one of the most important things to understand about OCD. Not because reassurance is wrong or because the people providing it do not care, but because in OCD, reassurance functions as a compulsion. And like all compulsions, it provides short-term relief while making the condition worse over time.
Understanding why this happens, and what to do instead, is often a turning point in recovery.
What Reassurance Seeking Actually Is
Reassurance seeking means trying to gain certainty or relief from anxiety by looking for confirmation that everything is okay.
In OCD, this can come from other people, from the internet, or from your own thoughts. It is one of the most common compulsions across all OCD themes, and one of the most frequently missed because it does not look like a ritual from the outside. It looks like asking a reasonable question. It looks like being careful. It looks like love.
Common forms of reassurance seeking in OCD include:
Asking a family member or partner repeatedly whether something bad will happen
Googling symptoms, information, or scenarios over and over to feel certain you are safe
Replaying a past event in your mind to confirm you did not cause harm
Asking for repeated confirmation about a relationship, a decision, or your own feelings
Confessing thoughts or actions to others to feel absolved of responsibility
Mentally telling yourself over and over that you are a good person or that nothing bad will happen
Checking your own body sensations or emotions repeatedly to see if they are 'right'
That last example is particularly important. Internal reassurance, the kind that happens entirely inside your own mind, is one of the most overlooked compulsions in OCD. Many people do not realize that silently repeating 'I would never do that' or mentally reviewing an event to confirm nothing went wrong is still a compulsion. It still feeds the cycle.
Reassurance seeking does not always look like asking for help. Sometimes it looks like thinking very hard. The mechanism is the same either way.
Why Reassurance Feels So Good in the Moment
Reassurance works in the short term because it genuinely reduces anxiety. When your mind is flooded with doubt and dread, hearing someone say 'you are fine' or finding an answer that confirms you are safe activates the same relief system in the brain as any other compulsion.
The nervous system calms down. The anxiety drops. And the brain records an important lesson.
The problem is that OCD's anxiety is not driven by real danger. It is driven by a misfiring threat system that is treating a harmless thought as an emergency. Reassurance reduces the alarm, but it does not fix the faulty system triggering it. In fact, every time reassurance successfully reduces the anxiety, the brain learns two things simultaneously:
That the threat was real enough to warrant a response
That reassurance is the correct and necessary tool for managing it
Over time, the brain becomes increasingly dependent on reassurance to feel calm. The threshold for what triggers the alarm gets lower. The amount of reassurance required to quiet it gets higher. What started as asking one question becomes asking the same question in five different ways. What started as one Google search becomes two hours of research that still does not feel like enough.
This is not a personal failing. It is a predictable neurological process.
The Reassurance Cycle in OCD
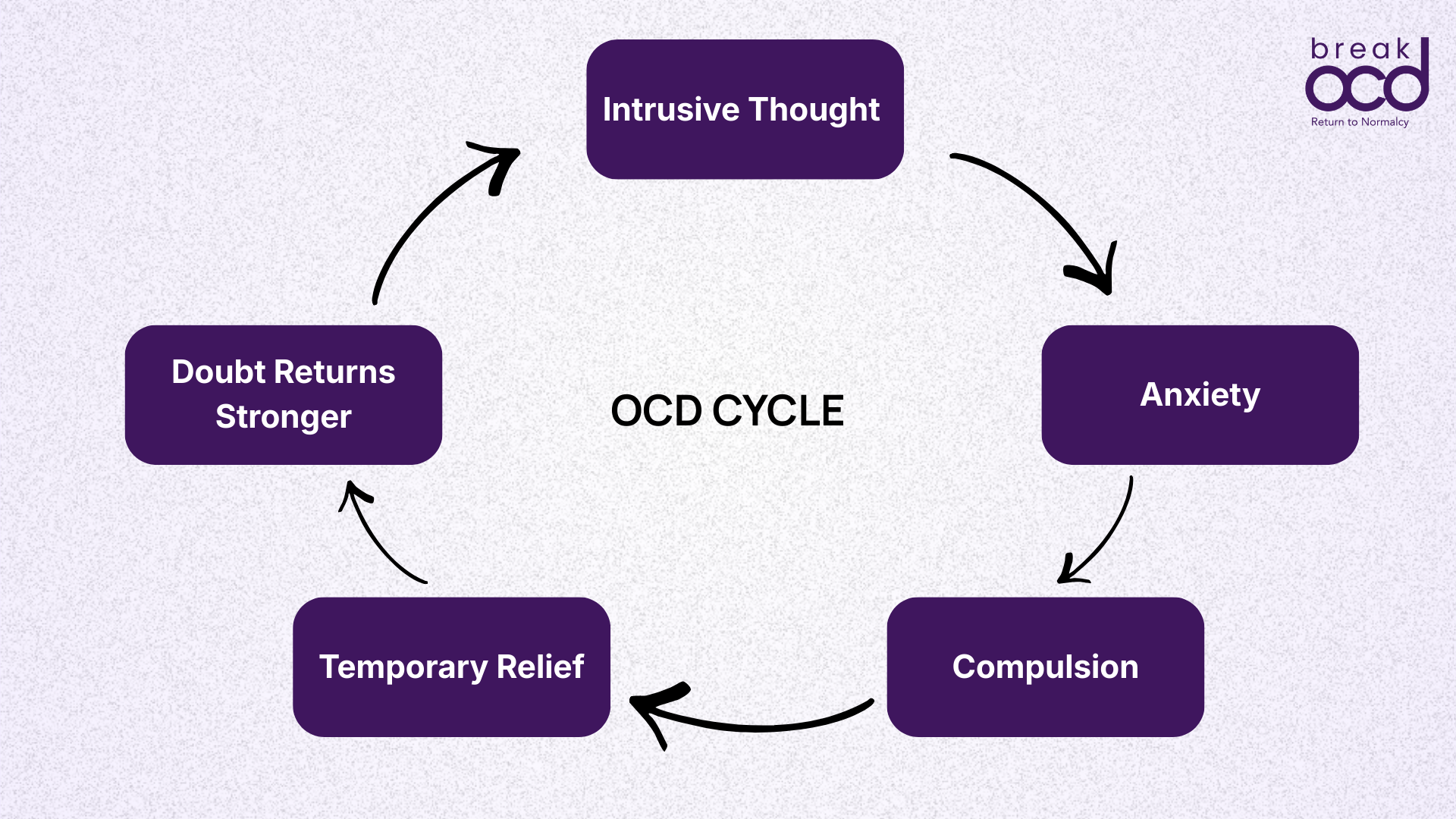
Reassurance follows the same cycle as every other compulsion in OCD:
An intrusive thought or doubt appears
Anxiety rises sharply
Reassurance is sought from a person, the internet, or your own mind
Anxiety drops temporarily
The brain learns that reassurance was necessary to feel safe
The doubt returns, often stronger than before
The urge to seek reassurance becomes more intense
The critical insight here is that the relief is real but the lesson is wrong. OCD is not teaching the person that the feared outcome did not happen. It is teaching them that safety only exists when certainty is achieved. And since complete certainty is never achievable, the brain will always find a reason to seek more.
This is why reassurance can feel like it is helping when it is actually making OCD stronger with every repetition.
The relief reassurance provides is not evidence that it is working. It is evidence that the compulsion is doing what compulsions do, which is reduce anxiety in the short term while reinforcing the cycle in the long term.
How Reassurance Seeking Shows Up Across OCD Themes
Because OCD attaches to what matters most to a person, reassurance seeking takes on different forms depending on the theme.
Harm OCD
Someone may ask repeatedly, 'You don't think I would ever hurt someone, do you?' or mentally replay every interaction from the day to confirm that nothing bad happened. The reassurance feels necessary because the fear of causing harm feels so real and so urgent.
Relationship OCD
A person may ask their partner again and again, 'Do you think we are okay?' or 'Are you sure you love me?' They may also spend hours internally checking their own feelings to see if they feel love strongly enough. In the context of arranged marriages, where families are involved and expectations are high, this form of reassurance seeking can become particularly distressing and difficult to identify as OCD rather than genuine relationship doubt.
Religious OCD
Someone may seek confirmation from a religious leader that a thought was not sinful, repeat a prayer until it feels perfectly right, or confess the same concern multiple times looking for absolution. In deeply religious Indian families, this can look indistinguishable from sincere faith, which makes it harder to recognize and harder to address.
Health OCD
A person may spend hours searching symptoms online, visit multiple doctors for the same concern, or ask family members repeatedly whether they look well. The internet in particular becomes an endless source of partial reassurance that never fully satisfies, because OCD always finds the one result that confirms the fear rather than the thousands that dismiss it.
Contamination OCD
Someone may ask whether a surface was clean, whether hands were washed properly, or whether a food item was safe. They may watch others complete cleaning tasks to confirm they were done correctly. What looks like reasonable caution is driven by an anxiety that no answer can permanently resolve.
The Indian Family Dynamic and Reassurance
This section is particularly important in the Indian context, because family structure in India creates a specific and very common reassurance pattern that is worth naming directly.
In Indian households, family members are deeply involved in each other's emotional lives. When a loved one is distressed, the instinct to help is strong and immediate. If a son asks his mother 'Are you sure nothing bad will happen to you?' the mother's natural response is to reassure him. If a wife is distressed about a thought she has had, her husband's instinct is to tell her she is a good person and she has nothing to worry about.
This is called family accommodation in clinical terms, and research consistently shows it is one of the strongest predictors of OCD severity and poor treatment outcomes. The more a family accommodates OCD through reassurance, the more entrenched the condition becomes, not because the family is doing something wrong, but because the reassurance is functioning as a compulsion even when it is given by someone else.
The person with OCD is not manipulating their family. They are genuinely distressed and genuinely seeking relief. The family is not enabling weakness. They are responding to real suffering with real love. The problem is structural, built into the way OCD uses certainty as a trap, and it requires a different kind of support to break.
Real support in OCD does not look like providing the answer the person is seeking. It looks like helping them sit with the uncertainty without responding to it.
In India, reassurance is often an act of love. In OCD, it is also an act that quietly maintains the condition. Families who understand this can become one of the most powerful parts of recovery.
The Difference Between Support and Reassurance
One of the most common fears people have when they learn about reassurance in OCD is that they cannot ask for any support or comfort at all. This is not true, and the distinction matters.
Reassurance in OCD attempts to eliminate uncertainty. It answers the specific feared question directly, confirming that the feared outcome will not happen.
Support helps a person tolerate uncertainty without needing to eliminate it. It acknowledges the difficulty without trying to resolve the doubt.
The difference in practice:
Reassurance sounds like: 'Nothing bad is going to happen, I promise you are fine.'
Support sounds like: 'I can see this is really hard right now. You can get through this.'
Reassurance answers the OCD question. Support acknowledges the person without answering the OCD question. Over time, support builds confidence and resilience. Reassurance builds dependence on certainty.
For families navigating this, the shift can feel cruel at first. Not providing reassurance to someone who is visibly distressed goes against every natural instinct. But learning to offer warmth and presence without providing the answer OCD is asking for is one of the most meaningful things a family member can do for someone with OCD.
Why the Brain Keeps Asking
People with OCD often describe a puzzling experience: they get the reassurance they were asking for, and it helps for a moment. Then a new version of the same question surfaces. Or the same question returns with a slight variation. No matter how many times the answer is given, it never feels like enough.
This happens because OCD is not actually asking a question that can be answered. It is generating doubt, and doubt by its nature cannot be resolved by certainty, only tolerated.
The mind keeps asking because OCD has learned that asking produces relief. The question is not really 'will something bad happen?' The question underneath is 'can I feel safe right now?' And because feeling safe through certainty is only ever temporary, the asking never stops.
This is also why the specific content of the question matters less than it seems. The theme may change. The feared outcome may shift. But the mechanism stays the same because it is not about the answer. It is about the anxiety.
What Actually Helps: Responding Differently
The goal of treatment is not to stop having doubts. Doubt is a normal part of being human. The goal is to change your relationship with doubt, so that it no longer demands a compulsive response.
Exposure and Response Prevention therapy, ERP, is the gold-standard treatment for OCD and works directly with reassurance seeking. In ERP, a person learns to:
Notice the urge to seek reassurance without acting on it
Allow the anxiety and uncertainty to exist without resolving them
Experience that anxiety naturally rises and then falls on its own, without the compulsion
Recognize that tolerating uncertainty is a skill that can be built over time
This is uncomfortable at first. The brain expects reassurance. When it does not arrive, anxiety spikes. This spike can feel like evidence that something is wrong. It is not. It is the brain's learned response to not getting what it has been trained to expect.
Over time, the urge weakens. The anxiety settles faster. The brain learns a new and more accurate lesson: uncertainty does not require certainty to be survived. You can tolerate not knowing, and life can continue.
That shift, from needing certainty to being able to live with uncertainty, is where real recovery begins.
Frequently Asked Questions
Is reassurance seeking always a compulsion in OCD?
Not every act of seeking reassurance is a compulsion. Asking for support, emotional validation, or practical advice in difficult situations is healthy and normal. In OCD, reassurance seeking becomes a compulsion when it is driven by OCD-related anxiety, when it targets the specific feared thought or outcome, and when the relief it provides is temporary and followed by a return of the doubt. The key distinction is whether the reassurance is aimed at eliminating uncertainty or simply receiving support.
Can reassurance seeking happen internally without asking anyone?
Yes. Internal or self-reassurance is one of the most common and most overlooked forms of reassurance seeking in OCD. It includes mentally replaying events to confirm nothing bad happened, silently telling yourself that you are a good person, checking your own emotions to see if they feel right, and reviewing past decisions for certainty. Because these behaviors are invisible, many people do not recognize them as compulsions at all.
Why do family members providing reassurance make OCD worse?
When a family member provides reassurance in response to OCD-driven distress, they are unintentionally performing the compulsion on behalf of the person with OCD. The relief the person feels is real, but it reinforces the OCD cycle in the same way that performing the compulsion themselves would. This is called family accommodation, and research consistently shows it is associated with more severe OCD symptoms and poorer treatment outcomes. Families who learn to offer support without providing direct reassurance become a significant asset in recovery.
What should I do when I feel the urge to seek reassurance?
The most effective response is to notice the urge without acting on it. This is easier said than done, especially at first. It helps to acknowledge the anxiety, remind yourself that the urge is a symptom of OCD rather than a signal of real danger, and allow the discomfort to exist without resolving it. Over time, with practice and ideally with the support of ERP therapy, the urge becomes less intense and easier to resist.
Does stopping reassurance seeking mean I can never ask for support?
No. The goal is not to become isolated or to suppress all emotional needs. The distinction is between support, which acknowledges your distress without answering the OCD question, and reassurance, which attempts to eliminate the specific uncertainty OCD is generating. You can absolutely reach out to someone when you are struggling. The key is in how they respond, and how you receive that response.
Sources & Further Reading
NHS: Obsessive Compulsive Disorder Overview
Government of India: Rights of Persons with Disabilities Act 2016